SPINE ENDOSCOPY
SPINE ENDOSCOPY
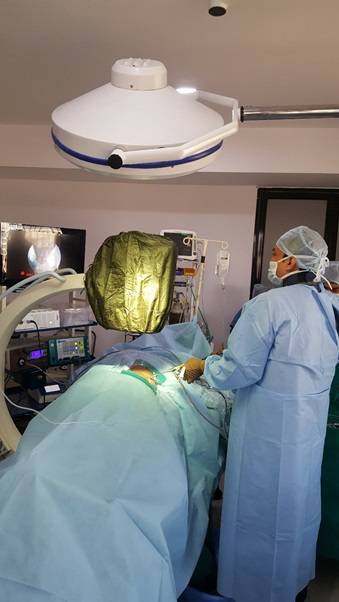
Lumbar Endoscopic Discectomy is a percutaneous alternative to open invasive surgery in patients with a herniated disc. Percutaneous surgery is performed through a needle puncture, as against a large incision in open surgery. The surgery is performed to remove the herniated disc, which has been exerting pressure on the spinal nerve and gives relief to patients suffering from lower back and leg pain. The surgery is performed through a small tube (trocar), which is inserted through the needle puncture, all the way to the disc. An endoscope inserted through the trocar allows the surgeon to see where the trocar is going and its surrounding areas. The procedure is performed under fluoroscopic guidance, which aids in the location of the herniated disc.
Lumbar Endoscopic Discectomy is a procedure to rectify herniated discs; however, not all patients with herniated discs require open discectomy procedure. Most patients get relief from non surgical treatments like anti-inflammatory medications, epidural injections, physical therapy and rest. But, in some patients the pain does not reduce despite medications and therapy. These patients may require a more aggressive intervention such as Lumbar Endoscopic Discectomy. A patient, who does not respond to nonsurgical treatment, may be asked to undergo a few diagnostic tests to verify the source of the pain. In case the diagnosis reflects a herniated disc, the doctor may recommend open discectomy.
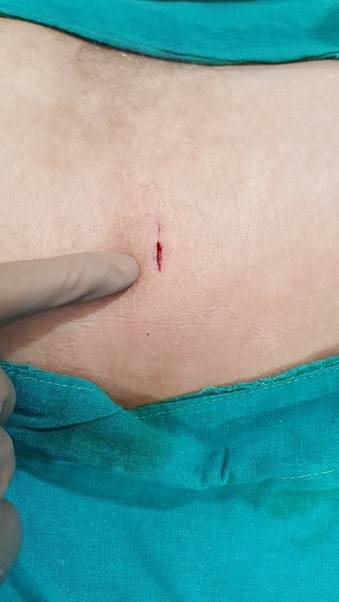
The patient is made to lie face down or on their side on the operating table. A mild sedative is administered to keep the patient relaxed throughout the procedure. A small incision is made on the skin over the back of the patient, just above the disc space. A needle is then placed through the incision and into the disc. Under fluoroscopic guidance, a small wire is then placed into the disc. The needle is exchanged for a series of small tubes, inserted through the same incision, over the guide wire. An endoscope and other special micro-surgical instruments are introduced through this tube and the segment of the herniated disc compressing the nerve is removed. The endoscope and intra-operative fluoroscopy guide the surgeon throughout the procedure. The tube and the endoscope are then withdrawn and the incision is closed. The procedure typically takes an hour to an hour and a half, depending on how many levels are being operated on. After the procedure the patient will require about two hours of post operative recovery time, before going home.
State of the art instruments are used in endoscopic surgery. The standard traditional surgical instruments have been miniaturized and elongated to fit through the endoscope. While specialized thermal probes are used to ablate diseased tissue, in some cases a laser is used to remove bone and disc. Despite the popularity of lasers in medical advertising; i.e. “laser surgery”; it is important to understand that the laser is simply a tool in the surgeon’s hand, and not the surgery itself.
Unlike traditional minimally invasive surgery, there is no need to strip any muscles from bone to access the spine; neither is there any need for any removal of healthy bones to access the spinal opening, nor are any spinal ligaments cut to access the disc. The small incision made on the skin, use of a needle to access the disc and the insertion of the needle through existing spinal openings; ensures that there is no damage to healthy tissues. This leads to a much quicker recovery for the patient.
Open discectomy has been performed over the course of the past 60 years and has improved and become more refined. Improved diagnostic tools—such as magnetic resonance imaging (MRI) and computerized tomography (CT) scans—allow physicians to gain a better understand of which patients will have the best results from the surgery.
The patient can go home within a few hours of the operation. Along with medication for pain, the patient needs to take rest for the first two or three days with some light stretching exercises. There should be a gradual increase in the activity levels over the next week, consisting of short walks initially and slowly returning to normal daily activities. The patient is advised to avoid any strenuous activity for a few months, including any activity which involves twisting of the torso. Physical therapy or chiropractic care can be resumed four weeks after the surgery. Since the procedure is minimally invasive, rehabilitation will generally be easier and faster than with traditional surgery. However, recovery time will vary based on individual factors.
Lumbar Endoscopic Discectomy is a relatively safe procedure. However, some of the risks associated with this surgery may include infection, bleeding, nerve damage and leakage of spinal fluid.
Located in Ahmedabad, LiveWell Pain Clinic brings you state-of-the-art procedure suite and high-tech operation theatre with the latest and best machines, devices and instruments, to ensure the highest standards and best results in your treatment. Offering in-house physiotherapy facilities along with all day care procedures, LiveWell Pain Clinic is the preferred choice of patient’s from India and countries like UK, USA, Tanzania, Russia, Kenya, among others.
Treating patients with back and neck pain, sciatic, frozen shoulder and trigeminal neuralgia, we at Live Well Pain Clinic believe in a compassionate patient-centric approach to offer effective long term relief from problems.